Calls for Lifestyle Modifications!
Your liver is the largest and the heaviest internal organ in your body. It helps process nutrients from food and drinks and filters harmful substances from the blood. By default liver cells contain a small amount of fat stored in them but if the amount of this fat increases beyond 5-10% of the actual weight of the liver (a little more than 3 pounds in an adult), it is termed fatty liver or hepatic steatosis.
Too much fat in your liver can cause liver inflammation, which can damage your liver and create scarring or cirrhosis, and in severe cases liver failure.
When fatty liver develops in someone who drinks a lot of alcohol, it’s known as alcoholic fatty liver disease (AFLD). In someone who doesn’t drink a lot of alcohol, it’s known as nonalcoholic fatty liver disease (NAFLD).
The incidence of NAFLD is more in the western world, nearly affecting about one-quarter of the population in the USA and Europe alone. It’s now becoming prevalent in India too due to a westernized lifestyle adaptation.
Fatty liver (NAFLD) is more of a lifestyle disorder
It’s more to do with our diet becoming more and more saturated with fats, refined carbohydrates, and abundant intake of aerated drinks that are full of fructose.
Insulin is a hormone that helps regulate the amount of sugar, or glucose (the end product of food degradation), in the blood. Fatty liver creates a condition called insulin resistance. This means that your body has enough insulin but is not able to use it properly. This leads to increased glucose in your blood. The liver turns this glucose into fat that accumulates in our liver.
Fatty liver is also increasing in incidence as a consequence of our reduced physical activity and our becoming slaves to gadgets, machines and vehicles, compromising our ability to burn off the fat.
What are the risk factors?
# The main risk factor for AFLD is drinking heavy amounts of alcohol.
The Center for Disease Control and Prevention (CDC) defines heavy drinking as – 15 or more drinks/week for men & 8 or more drinks/week for women
In addition to heavy alcohol consumption, other risk factors for AFLD include:
- obesity
- smoking
- older age
- genetics
- history of certain infections, such as hepatitis C
# The major risk factors for NAFLD are:
- overweight or obesity
- insulin resistance
- type 2 diabetes
- high levels of fat, especially triglycerides in the blood
- metabolic syndrome
- having a family history of liver disease
- side effects of certain medications such as methotrexate (Trexall), tamoxifen (Nolvadex), and amiodarone (Pacerone)
- pregnancy
- infections, such as hepatitis C
- polycystic ovary syndrome (PCOS)
- obstructive sleep apnea
- exposure to certain toxins
- rapid weight loss
- rare genetic conditions, like Wilson disease or hypo beta lipo proteinemia
Having risk factors means you’re at an increased risk of fatty liver disease compared with people who don’t have risk factors. It does not mean you’ll certainly develop it in the future.
If you have one or more risk factors for fatty liver disease, talk with your doctor about prevention strategies.
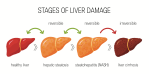
Stages of fatty liver
Fatty liver can progress through four stages:
- Simple fatty liver. There’s a buildup of excess fat in the liver. Simple fatty liver is largely harmless if it doesn’t progress.
- Steatohepatitis (NASH). In addition to excess fat, there’s also inflammation in the liver.
- Fibrosis. Persistent inflammation in the liver that has caused some scarring. However, the liver can still generally function normally.
- Cirrhosis. Scarring of the liver has become widespread, impairing the liver’s ability to function. This is the most severe stage and is irreversible.
Symptoms of Fatty Liver
In most people, there are hardly any symptoms. They come to know about the presence of fatty liver during a routine USG or while undergoing investigations for some other problem. In others, there are some vague and generalized symptoms. Only in advanced cases where liver cirrhosis has set in, do the symptoms become pronounced. Following are the symptoms of fatty liver one may experience –
- generalized fatigue and weakness
- loss of appetite in some
- slight pain in the right side of the abdomen
- nausea and vomiting in a few
- redness of the palms
- jaundice with yellowness of skin and eyes may be present in advanced disease
How is fatty liver diagnosed?
# Physical examination
If your liver is enlarged, your doctor might be able to feel it on a physical examination. Your spleen may also get enlarged and palpable.
# Blood tests
- Liver function test: Liver enzymes SGOT, SGPT, AST or ALT may be elevated as a sign of liver inflammation.
- Lipid profile: Triglyceride levels may also be on the higher side.
# Imaging
- Abdominal ultrasound is often the initial test when liver disease is suspected.
- Computerized tomography (CT) or magnetic resonance imaging (MRI) of the abdomen, though lack the ability to distinguish NASH from NAFLD, may still be used.
- Transient Elastography is an enhanced form of ultrasound that measures the stiffness of your liver. Liver stiffness indicates fibrosis or scarring.
- Magnetic resonance elastography works by combining MRI imaging with sound waves to create a visual map (elastogram) showing the stiffness of body tissues.
# Liver biopsy
Is generally done to evaluate the presence and extent of scarring in your liver if other tests are inconclusive. It can be uncomfortable and does have small risks that your doctor will review with you in detail. The procedure is performed by a needle insertion through the abdominal wall and into the liver to draw a sample of the liver tissue.
Is Fatty liver reversible?
Currently, hardly any specific medicine has been approved to treat fatty liver disease. Thus it’s possible for the damage caused by fatty liver disease to be reversed only when addressed in the early stages. The primary treatment for fatty liver disease focuses on lifestyle and dietary changes that promote liver health.
Lifestyle changes
Lifestyle changes are the first line of treatment for fatty liver disease. Depending on your condition and lifestyle habits, it might help to:
- lose weight, especially abdominal fat. Losing around 10% of one’s body weight can improve the condition.
- reduce or abstain from alcohol consumption.
- get at least 30 minutes of exercise most days of the week
- avoid medications and supplements that are hard on your liver
- protect your liver health from viral infections through vaccines for hepatitis A and hepatitis B and regular screenings for hepatitis C.
- vitamin E supplements might help improve ALT and AST levels, inflammation, and excess fat in NAFLD.
Dietary modifications
The following dietary changes might help manage your fatty liver disease and lower the risk of complications:
- Balance your diet. Try to select foods from all food groups. This includes fresh fruits and vegetables, whole grains, lean proteins, low-fat dairy, and healthy fats and oils.
- Cut calories. Aim to limit your consumption of foods that are high in calories.
- Focus on fibre. Increase intake of foods that are rich in fibre – fresh fruits and vegetables, legumes, and whole grains. Fibre can help improve the function of your liver.
- Limit certain foods. Take steps to reduce your consumption of foods that are high in:
- refined carbohydrates, such as sweets, white rice, white bread, or other refined grain products
- saturated fats, which are found in foods such as red meat, full-fat dairy, and fried foods
- trans fats, which are present in fried foods and many processed snack foods
- Increase intake of Omega-3 fatty acids and monounsaturated fats. Fish, nuts, flaxseed, olives and green leafy vegetables are rich sources. Increasing the intake of these fats in your diet can help your body use the available insulin in a better manner.
- Avoid raw or undercooked shellfish. Raw or undercooked shellfish can contain bacteria that can make you seriously ill.
- Drink water. Drinking plenty of water can help keep you hydrated and also improve your liver health.
Homoeopathy for fatty liver
Homoeopathy has some very specific medicines for the treatment of fatty liver. They not only act on the disease process affecting the liver but also treat the patient holistically on their symptom totality. Here’s a short list of the 5 best homoeopathic medicines for fatty liver based on the individualizing symptoms given by the patients for an effective and holistic recovery.
5 best Homeopathic medicines for Fatty Liver
- Chelidonium: is one of the best homoeopathic medicines for the fatty liver with pain under the right shoulder blade.
- Lycopodium: fatty liver with fullness of the stomach and sour eructations immediately after eating just a few mouthfuls.
- Nux Vomica: when a highly sedentary lifestyle, abuse of stimulants such as tea, coffee and alcohol over a period of time contributes to fatty liver.
- Phosphorus: fatty liver in usually tall and skinny people with increased thirst and intolerance to warm water/drinks, which are vomited out as soon as they become warm in the stomach.
- Calcarea Carb: fits in well for fatty liver in obese people. There is a strong craving for indigestible things like chalk, earth or pencils with prominent heartburn and loud belching.
Do visit your Homoeopathic Physician if you happen to get diagnosed with the above-discussed condition. It’s possible for the damage caused by fatty liver disease to be reversed when addressed in the early stages...