Are you suffering from a painful lump on the butt? Is the sight of blood in the toilet bowl or tissue paper frightening? Well, do not panic, it is probably a hemorrhoid/pile. It can be distressingly painful and might make sitting down, an activity that comes last in your wish list, but it’s curable.
What are hemorrhoids?
In their normal operational state, hemorrhoids (also referred to as piles or बवासीर) are blood vessels that convey blood to the lower rectum and anus. Although thought of as unpleasant inflammations, they are actually a normal part of our anatomy and are located at the junctions where small arteries merge into veins and are cushioned by smooth muscles and connective tissue. When these hemorrhoids become too big, clogged or swollen (inflamed/varicosed), is when the trouble occurs and they are called piles or pathological hemorrhoids.
They are most common among adults aged 45-65. This does not mean, however, that young people and children do not get them. They are much more common among men than women. A woman is most likely to get them when she is pregnant.
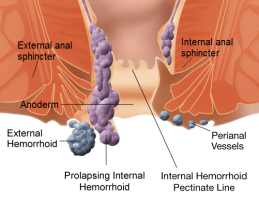
They can be of various sizes and may be internal (inside the anus) or external (outside the anus). Typically, internal piles occur from 2 to 4 cm above the opening of the anus while external piles occur on the outside edge of the anus. Both can occur at the same time but the internal ones are much more common.
Why do hemorrhoids occur?
Hemorrhoids are caused by swelling of the veins in the anal canal. The exact cause is unclear, but they are associated with increased pressure in the blood vessels in and around your back passage. Conditions that might increase your risk of developing them are:
- too much straining at stools due to prolonged constipation or diarrhea
- regular postponement of bowel movement causing drying up and hardening of feces within the intestines
- unhealthy diet consisting of processed foods, refined flours, animal proteins and sugar that are low in roughage
- Increased use of alcohol and caffeine
- pregnancy
- regularly lifting heavy objects
- a persistent cough or repeated vomiting
- sitting down for long periods of time
- being overweight or obese
- anal intercourse
The tendency to develop hemorrhoids may also be inherited. The risk of developing them grows with age as your body’s supporting tissues get weaker.
What are the symptoms?
The most common symptom of Internal hemorrhoids – the small swollen veins in the wall of the anal canal – is painless bright red blood covering the stool or on toilet paper or in the toilet bowl. However, if an internal hemorrhoid gravitates/protrudes through the anus outside the body, it can additionally cause –
- an itchy bottom
- pain while defecating and also while cleaning up
- a lump hanging down outside of the anus, which may need to be pushed back in after passing a stool
- difficulty in passing out stool either as a result of intense pain or itching around the anal area or bulging swollen veins which prevent smooth bowel and muscle movement.
- mucus discharge after passing a stool, staining your underclothes
- soreness, redness and swelling around your anus
- feeling of fullness in the bowels and an urge to pass out stool again even after an evacuation due to the bulging hemorrhoid pressing at the anus
- leakage of feces due to failure in the normal functioning of the muscles around the anal area.
Internal hemorrhoids are classified into four grades:
- Grade 1 – are small inflammations that usually remain inside the lining of the anus and are not visible
- Grade 2 – are larger than grade 1 hemorrhoids, but also inside the anus. When passing a stool, they may get pushed out, but return unaided
- Grade 3 – also called ‘prolapsed hemorrhoids’, bulge outside the anus. You may feel them hanging out but they can be pushed back in with a finger
- Grade 4 – are large and stay outside the anus all the time. They cannot be pushed back in and need to be treated by a doctor.
External hemorrhoids can be felt as a small bulge in/around the anus. They are very itchy but can get painful if a blood clot forms inside them. In such cases a hard lump blue or yellow may be felt around the anus called a ‘thrombosed external hemorrhoid’. It would require medical treatment straight away.
Complications linked to hemorrhoids
- Hemorrhoids aren’t usually painful unless their blood supply slows down or is cut off. When the blood supply to an internal hemorrhoid gets interrupted, it results in a strangulated hemorrhoid causing severe pain, or even gangrene (death of tissue) and require emergency treatment.
- They can sometimes cause long-term blood loss, which may lead to anemia.
How do we diagnose them?
We doctors may ask you several questions like – “Do any of your close relatives (parents, siblings) have piles?”, “Has there been any blood or mucus in your stools?”, “Has there been any recent weight loss?”, “Have your bowel movements changed recently?” or “What color are your stools?”, etc etc.
A doctor can usually diagnose piles after carrying out a physical examination i.e examining the patient’s anus. For internal hemorrhoids, he or she may perform a digital rectal examination (DRE) or use a proctoscope – a hollow tube fitted with a light that allows the doctor to see the anal canal. The doctor may also take a small tissue sample from inside the rectum and send it to the lab for analysis to exclude other disease conditions.
What are the available treatments?
The first thing that people do to cure hemorrhoids is get an OTC (over-the-counter) medication, without knowing their possible side effects. Many of these ointments, creams, pads etc. contain witch hazel, hydrocortisone, or some other active ingredient which can relieve symptoms of swelling, itching or pain. But its important to remember that they do not cure piles, they only treat the symptoms. Moreover longer periods of usage may irritate the anus area and cause skin thinning.
Corticosteroids too can reduce inflammation and pain but long term use is not advisable.
Painkillers or laxatives have very temporary effects and in fact do more harm in the long run.
Procedural options
Various procedural options are available like – Infrared coagulation for grades 1-2, Banding or ligation or Sclerotherapy for grades 2-3 and surgical options like Hemorrhoidectomy or Hemorrhoid stapling for large internal hemorrhoids (grades 3 or 4) if above procedures prove ineffective.
All these procedures are done on an outpatient basis which means that you go home after the procedure, but they come with their own set of complications and do not guarantee a non-recurrence.
How can you prevent them?
Some simple lifestyle modifications can help you prevent or even cure piles. Take ‘a softer stool’ and ‘regular bowel movement’ as your main goals.
- High-fiber diet – If your piles are a result of constipation, a change in diet can help keep the stools regular and soft. Eat more fiber, such as fruit and vegetables, or switch your cereal breakfast to bran. Fiber supplements such as Psyllium Husk can add to the bulk.
- Increase fluid intake – Water is the best drink. Increase your water consumption to at least 6-8 glasses a day.
- Drink chamomile tea several times a day. Avoid too much caffeine
- Do exercise – Shed those extra pounds.
- Never hold in stools – it can cause irregular bowel movement and hardening of the stools.
- Try not to strain when you go to the toilet – it may cause your rectal veins to swell.
Self care tips for piles
- Warm sitz bath helps to relieve pain and relax the engorged and clogged veins.
- Cold compresses help to reduce pain, itching and also shrink hemorrhoids by constricting blood vessels.
- Hydration – Dryness may aggravate hemorrhoids and may cause excessive bleeding. Never use a dry tissue to wipe the affected area as it may cause unwanted scratches that can worsen the swollen vessels. Applying extract from vitamin E capsule in and around the anal area can soothe and re-hydrate it.
- Topical application of soothing agents (like honey, aloe Vera, tea tree/olive oil) help.
- Avoid wearing tight under clothes to avoid unnecessary friction
Get hemorrhoid-free with Homoeopathy
Homeopathic Remedies for hemorrhoids aim at correcting the internal disturbances of venous system. They make the vein valves stronger thus preventing the blood to stagnate in them. This helps in a complete recovery for you. Homoeopathy should be the preferred, in fact, the first mode of treatment in piles. The sooner you approach a homeopathic physician for piles treatment, higher are your chances of a complete recovery and avoidance of surgery. Homoeopathy can proudly boast of having innumerable number of remedies for all kinds/degrees of piles. Medicines like Aesculus, Aloes, Collinsonia, Hammamelis, Muriatic acid, Nitric acid, Nux vomica, Paenoia, Ratanhia, Millifolium, Ficus, Phosphorus and Thuja are a few of the many that not only take care of the pain and bleeding but also act on your varicosed rectal veins and strengthen them to bring about a lasting cure in the most harmless, safe and gentle way without any side effects. When given on your individualizing symptoms and constitution, a single Homoeopathic remedy is power packed to take care of all your distress in a short duration of time.
Do give Homoeopathy a try before going under a ‘Surgeon’s Knife’ to avoid complications and a recurrence.

