“Hi Doc, I’m miserably anxious! I haven’t slept in days; some days, I feel extremely restless n snappy, and I’m so dull, gloomy and weepy on others. I don’t know what’s happening to me… am I going crazy? Do you have some solution?” enquired a 48-year-old who visited my chamber about two months ago. Her confident voice echoed loud n clear, audible to the patients in waiting. She was either taking in deep breaths or yawning constantly. “I’m missing my periods… I’m so burpy n uncomfortable all the time… I feel suffocated… I can’t focus.. my work is suffering. Will I ever be my normal again??”
The Menopause or Climacteric Phase in the ageing of women is a natural biological process, marking the transition from a reproductive phase to a non-reproductive state; wherein a woman’s menstrual periods stop permanently, the function of her ovaries ceases and she is no longer able to bear children. Medically speaking the transition is complete when there’s an absence of menstrual periods for 12 or more months.
Why does it happen?
The ovaries, about the size and shape of an almond, are a pair of reproductive glands in women located in the pelvis, one on each side of the uterus. They produce ova or eggs and are the main source of synthesis of two female sex hormones –
- Estrogen is a by-product of the maturation of the egg, and
- Progesterone is produced by the corpus luteum (a follicle or sac) in the ovary following the release of egg (ovulation).
These hormones are crucial for the development and smooth functioning of the female sexual reproductive system, as in –
- the development of female body characteristics such as the breasts, body shape, and body hair
- regulate the menstrual cycle
- pregnancy
- estrogen also protects the bones
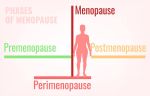
Different stages of menopause
Peri-menopause: Also known as menopausal transition, is the “time around menopause” and spans between 4-7 years for women. During this period, women start experiencing irregular menstrual periods along with various other symptoms.
Pre-menopause is the time closer to but before menopause.
Menopause is the absence of menstrual periods for one full year.
Post-menopause refers to the time after menopause has occurred.
The age at which a woman typically reaches menopause
The average age of menopause is 50 years. Most women reach menopause between the ages of 45 and 55, but it may occur as early as in the age of 30s or 40s, or may not occur until a woman reaches her 60s.
There is no specific way to predict when an individual woman will have her menopause or begin having symptoms suggestive of menopause, but the total fertility period in a female is approx. taken as 30 years, so we can add that to her age of menarche or first period; to get a rough estimate.
There is no reliable lab test to predict when a woman will experience menopause. As a rough “rule of thumb,” women tend to undergo menopause at an age similar to that of their mothers.
Early menopause – external conditions that can affect the timing of menopause
Certain medical/surgical conditions and lifestyle choices can influence the timing of menopause.
- Surgical removal of ovaries – oophorectomy – in an ovulating woman will result in immediate menopause called surgical or induced menopause. In this case, there is no peri-menopause. After the surgery, in the absence of ovaries, there is a sudden and complete drop in hormone levels.
- After Surgical removal of the uterus – hysterectomy, women often report an abrupt and acute onset of severe menopausal symptoms (though not always), when the ovaries are removed together with the uterus – Pan Hysterectomy or subtotal hysterectomy. (HRT helps in such cases).
- If a hysterectomy is performed without removal of both ovaries in a woman who has not yet reached menopause, the remaining ovary/ovaries are still capable of normal hormone production. Though the woman won’t be able to menstruate after the uterus is removed, it won’t be called “true” menopause as the ovaries may still continue to produce hormones up until the normal time when menopause would naturally occur. These women could then experience the other symptoms of menopause such as hot flashes and mood swings around their natural age of menopause, though they cease to menstruate immediately after the surgery.
- Premature ovarian failure is the occurrence of menopause before the age of 40. The condition occurs in about 1% of women worldwide. The cause of premature ovarian failure is not fully understood, but it may be related to – a) autoimmune diseases such as hypothyroidism, Graves’ disease, lupus or due to genetic factors, b) It can occur as early as 1 to 2 years following a hysterectomy, perhaps due to a compromised blood supply to the ovaries. c) Related to Cancer chemo and radiation therapy, depending upon the type and location of cancer and its treatment. The symptoms may begin during/following the cancer treatment.
- Lifestyle choices like excessive smoking or stress may induce it.
What are the symptoms of menopause?
Women experience most of the physical and psychological symptoms in the peri-menopausal stage. As mentioned earlier, a sudden drop in the female sex hormones is the cause of the multiple bodily changes that one experiences during this phase of life.
It’s a different and individual experience for each woman. Some may experience few or no symptoms, while others can experience multiple physical and psychological symptoms.
The extent and severity of symptoms can also vary significantly. They may come and go over an extended period for some women which too, is highly individual.
# Changes In The Menstrual Cycle
One of the early signs of identifying menopause is an irregular menstrual cycle in terms of length, flow and frequency. Women will start getting less frequent periods. There can be various extremes, either scanty bleeding, spotting or heavy bleeding. Doctors use terms like amenorrhea, oligomenorrhea, menorrhagia and metrorrhagia depending upon the pattern.
This menstrual irregularity is also associated with a decrease in fertility since ovulation becomes irregular and there might be anovulatory cycles too. However, one may still become pregnant until they’ve reached true menopause and should still use contraception if they do not wish to become pregnant.
# Other Common Physical Effects Of Menopause:
- Hot flashes or a sudden feeling of intense heat not caused by external sources. These usually last from 30 seconds to several minutes (less than 10) and may go on for as long as 5 to 10 years.
- Flushing or reddening of the face and upper body.
- Drenching night sweats might necessitate one to get out of bed several times during the night – to open a window, take a shower, change clothes or maybe change the bed linen too!! This scenario can occur every single night… over many weeks, months and sometimes years!!
- Wakefulness or sleeplessness consequent upon hot flashes or night sweats, with daytime tiredness.
- Headaches or migraines.
- Vaginal atrophy and dryness might lead to painful coitus and an increased risk of vaginal infections.
- An increased risk of urinary tract infections particularly cystitis, feeling the need to urinate more frequently, urinary incontinence, or even stress incontinence.
- Decreased libido or sex drive.
- Changes in skin texture, including wrinkles, warty excrescences and skin tags, hypo or hyperpigmentation, adult acne, dryness of skin, hair and nails.
- Some amount of hair thinning or hair fall.
- Hirsutism or increased hair growth on areas like the face, chin, and neck.
- Sore and tender breasts. Also, there is a reduction in the amount of glandular tissue in breasts with an increase in fat deposition.
- Some degree of weight gain; though the distribution of body fat may change with body fat being deposited more in the waist and abdominal area than in the hips and thighs. These extra pounds on the waistline might lead to a greater chance of heart disease.
- Painful or stiff joints. Osteoporosis, a deterioration of the quantity and quality of bone, causing an increased risk of fractures is a consequence of both age and hormonal changes during menopause.
# A drop in the sex hormones impacts the mental health of women too, which may cause them to experience:
- Anxiety
- Depression
- Indecisiveness
- Irritability
- Difficulty to concentrate
- Memory loss
How does one recognize the onset of menopause?
If you are missing your periods or experiencing any other irregularity in your cycle, it is best to visit your doctor to get a few tests done.
The only way to diagnose menopause is –
- The lack of menstrual periods for 12 months in a woman in the expected age range.
- Declining levels of female sex hormones. In women without a uterus, menopause or post-menopause is identified by very high levels of FSH.
- Repeated USG over the year may show a gradual thinning of endometrial tissue indicating approaching menopause.
How can you prepare for menopause?
A woman’s body undergoes sudden, drastic and harsh physical and psychological changes during menopause. The declining hormones also affect other parts of the body, especially the bones and the heart. However with awareness, appropriate and timely medical intervention, and diet and lifestyle changes, women can take care of themselves.
Available treatment options for menopause
Menopause is a normal ageing process and not a disease that requires treatment. However, treatment of associated symptoms is possible if they become substantial or severe.
1. Hormone therapy (HT) or hormone replacement therapy (HRT) or postmenopausal hormone therapy (PHT) helps in controlling the symptoms of menopause related to declining estrogen levels such as hot flashes, night sweats, sleep disturbances, psychological and genitor-urinary issues like urine frequency and vaginal dryness and prevention of osteoporosis. These are synthetic hormones made in a lab that are chemically identical to the hormones in our body and consist of a) estrogen or b) a combination of estrogen and progesterone (progestin). They are available in oral (pill) and transdermal (patch and spray) forms.
Awareness and use of HRT are more prevalent abroad than in India as it is not a preferred mode of treatment here. If anyone still wants to go for it, it’s better to be aware of the risks involved.
- Transdermal hormone products are already in their active form without the need for “first pass” metabolism in the liver to be converted to an active form. Since they do not have effects on the liver, this route of administration has become the preferred form for most women. They are administered transdermally as creams or gels.
- Women receiving combined hormone therapy with both estrogen and progesterone have an increased risk of heart attack, stroke, and breast cancer (75% more) when compared with women who did not receive HT.
- Studies of women taking oral estrogen therapy alone show an increased risk for stroke, but NOT for heart attack or breast cancer (if used for less than 10 years). But estrogen therapy alone is associated with an increased risk of developing endometrial cancer* in postmenopausal women who have not had their uterus surgically removed since oestrogen stimulates the hypertrophy and hyperplasia of the uterine wall if given alone without progesterone, so the risk of cancer.
**It is recommended that if hormone therapy is used, it should be used in the smallest effective dose for the shortest possible time.
**It should be only used if the balance of risks and benefits is favorable for the individual woman.
**Women on HRT should be re-assessed by their doctor at least annually.
2. Oral contraceptive pills: Some women tend to have considerable breakthrough bleeding when given estrogen therapy during the menopausal transition. Therefore, oral contraceptives are given to them to regulate menstrual periods, relieve hot flashes, as well as to provide contraception.
3. For symptoms of vaginal estrogen deficiency, the available local hormone and non-hormone treatments are –
- Hormonal: Vaginal estrogen ring (Estring), cream, or tablets.
- Non-hormonal: Moisturizing creams or lotions – K-Y Silk-E vaginal moisturizer or KY Liquibeads vaginal moisturizer or lubricants for managing the discomfort of vaginal dryness. Soaking in a sitz bath or a bathtub of warm water may help relieve symptoms of burning and vaginal pain after coitus.
- Homoeopathic – Calendula and Hydrastis in gel form or tincture in sitz bath work wonders in such cases.
4. Antidepressants may be prescribed by your doctor but they come with their side effects, including decreased libido or sexual dysfunction.
Homoeopathy Helps
Listing a few homoeopathic remedies that give excellent results and make this critical phase comfortable for women. Each medicine defines a constitution and provides a holistic treatment involving both body and mind rather than treating a few symptoms alone.
Lachesis: The woman gets melancholic, irritable, always restless and suspicious, with religious insanity. Very talkative, or sad with no desire to mix with the world. Dark-coloured haemorrhage from the uterus. Menses are short and scanty. All troubles are relieved greatly by the menstrual flow. Excellent remedy for hot flashes, distressing headaches, palpitations and haemorrhoids. Sleeps into an aggravation. Always better after the period.
Sulphur: Menopause changes the constitution and one seems to be losing weight even with a good appetite. Looks lean, thin, stoop-shouldered with intense burning/hot flashes. Becomes forgetful, irritable, depressed and delusional. Menses too late, short, scanty, acrid with soreness. Skin is rough, dry, dirty and itchy. Discharges are offensive and acrid making all body orifices red. Catnap sleep.
Calcarea Carb: Menses too early, too profuse and too long-lasting turning one pale and anaemic. Suited to fair, fat and flabby women in a mentally or physically jaded state due to overwork. Profuse cold, damp and sour sweat particularly around the head wetting the pillow, causing wakefulness.
Pulsatilla: Though a remedy well known for its effects during puberty, given the mental state, even menopausal women respond very well to it. Mild, gentle, yielding women with a weepy disposition, crying readily. Changeable temper with delayed, suppressed and scanty menses. Flow being thick, dark, clotted, changeable and intermittent. Feels suffocated in a closed warm room with hot flashes. Better open air.
Sepia: Tall, thin, easily depressed women who suddenly turn indifferent to their loved ones. Irritable, and weepy while telling symptoms, they dread being alone and are anxious towards evenings. Periods too late, scanty, irregular with hot flashes.
Actea Racemosa: Suited to rheumatic, nervous women with ovarian irritation, uterine cramps and heavy limbs. Rheumatism affects the belly of large muscles. Violent headaches. Irregular, profuse, dark, clotted and offensive periods with back aches. Ovarian pains felt from hip to hip. Menses is the worst time; the more profuse the flow, the greater the suffering.
Platina: Mental troubles associated with suppressed menses. Physical symptoms disappear as mental symptoms develop. Arrogant and proud women with contempt for others. Excessive bleeding of dark clotted blood with pain in ovaries. Nymphomania. The medicine is highly effective in treating dyspareunia (painful sex) due to the hypersensitiveness of parts.
Lifestyle Management in Menopause
Apart from medication, many of the symptoms of menopause and medical complications that may develop in postmenopausal women can be lessened or even avoided by making conscious efforts to lead a Healthy Lifestyle:
- Regular exercise can help protect against cardiovascular disease as well as osteoporosis. In addition, it also has known mental health benefits. Yoga helps build physical and mental health too.
- Proper nutrition: Diet rich in plant estrogens (phytoestrogens, isoflavones) – soybeans, chickpeas, and lentils have a chemical structure similar to the estrogens naturally produced by the body. These may help relieve hot flashes and other symptoms of menopause particularly in women who have had breast cancer and do not want to take hormone therapy (HT) with estrogen. Foods like cabbage, soy products, red fruits and vegetables like apples, oranges, cherries, strawberries, beetroots, red bell pepper, tomatoes, beans, carrots, flaxseeds and walnuts, olives, avocado oil etc. act as anti-ageing foods that increase collagen.
- Vitamin E supplements provide relief from mild hot flashes, but one has to be careful with the dosage as taking a dosage greater than 400 international units (IU) of vitamin E may be associated with cardiovascular disease risk.
- Cutting down on smoking, caffeine and alcohol will reduce the risk of cardiovascular disease.
- Late-night/wee-hours prowling around the house due to reduced sleep can be calmed with hormone replacement therapy (HRT) – but it’s not for everyone. Homoeopathic treatment can help you avoid sleeping pills.
- For urinary frequency and incontinence, there are exercises, medications and behavioural techniques that can re-train those weakened muscles. All of which are better ideas than staying home to avoid public embarrassment.
- To reduce the soreness/pain in the breasts one can cut down on caffeine and fat intake, and apply a cold or hot compress. It may help to wear a sports bra during the day or while sleeping for extra support.
- For osteoporosis, our long-term goal is the prevention of bone fractures in future by slowing bone loss and increasing bone density and strength. Although early detection and timely treatment can substantially decrease the risk of fractures, none of the available treatments for osteoporosis is a complete cure. Lifestyle changes like abstaining from cigarette smoking, curtailing alcohol intake, exercising regularly, and consuming a balanced diet with adequate/fortified calcium and vitamin D or taking Calcium and vitamin D supplements help. Your doctor might prescribe medications that stop bone loss and increase bone strength like calcitonin (Calcimar). There are several Homoeopathic medicines to increase bone density and strength.
All is NOT Gloomy…
You are not alone in this. Every woman will experience menopause in her life, sooner or later. Though the symptoms may appear burdensome, there is a feel-good factor too…
In some women, medical issues like endometriosis or uterine fibroids might in fact improve after menopause due to regression.
Menopause is your freedom phase, your HAPPY PERIOD ladies! Your career is at its peak, your family responsibilities are coming to an end, your busy schedules and hectic lifestyle with young children to bring up are already done with… and most importantly, the constant tension of an accidental pregnancy is also over!!
Happiness is the key to good health. Age gracefully and take good care of yourself. After all, menopause is just another stage of life!!
Is there a Male Menopause too?
Yes, there is – Andropause. TBD some other time…