The term ‘epilepsy’ comes from a Greek word, meaning ‘to take hold of’, and hence the use of the term ‘seizure‘- to seize, to describe its effects.
If you’re living with a seizure disorder, it can get in the way of life, especially, if the fits keep recurring.
I know of a teenager who would get fits at the least excitement. At her 12th Conti Party – a continuation of the school farewell celebrations – by the poolside, she suddenly got a seizure attack, fell into the empty pool and broke her lower front teeth!! In another instance, a 23-year-old college-goer got his first seizure attack while driving and straightaway hit a tree. Luckily, no one got injured..
These episodes do make one get anxious or stressed about what the future holds. They affect one’s mental health and may bring in fear, anger, aggression, rebel, lack of confidence or mere listlessness and no desire to do anything.
It’s important to talk with your health care professional and seek ways to help equip you better in managing or controlling your seizures, thus feel better and have a more active and full life.
Know When To Visit Your Doctor
Seek immediate medical help if:
- The seizure lasts more than five minutes.
- Breathing or consciousness doesn’t return after the seizure stops.
- A second seizure follows in immediate succession.
- You have high fever.
- You’re experiencing heat exhaustion.
- You’re pregnant.
- You have diabetes.
- You’ve injured yourself during the seizure.
If you’re experiencing a seizure for the first time, it’s an absolute must to seek medical advice.
Prepare For Your Appointment
In a few cases, seizures need immediate medical attention and there is no time to prepare, while in others, your first appointment to evaluate the seizure can be with your family doctor, or you may be referred to a neurologist, or an epileptologist (a doctor trained in epilepsy).
To prepare for your appointment consider what you can do to get ready, and understand what to expect from your doctor.
What you can do
- Record information about the seizure. Include the time, location, symptoms you experienced and how long they lasted (if you know these details).
- Be aware of any pre-appointment restrictions. At the time you make the appointment, ask if there’s anything you need to do in advance to be ready for any medical tests.
- Write down key personal information, including any major stress or a recent life change.
- Make a list of all medications, vitamins or supplements that you’re taking, including dosage.
- Take a family member, friend or coworker along who was a witness to your episode to help fill in all the necessary information.
- Write down questions to ask your doctor, to help make the most of your time with the doctor.
What to expect from your Doctor
Your doctor is likely to ask you several questions:
- Can you describe your seizure episode?
- Where were you and what happened right before it started?
- Was anyone there to witness what happened?
- What do you remember feeling just before or right after the seizure?
- What symptoms did you experience?
- How long did the seizure last?
- Have you ever had a seizure or other neurological problem in the past?
- Do you have any family members diagnosed with a seizure disorder or epilepsy?
- Have you recently travelled outside the country?
Lifestyle Modifications
Some steps you can take to help with seizure control:
- Take medication correctly. Don’t re-adjust the prescribed dosage without consulting your doctor.
- Get enough sleep. Lack of sleep can trigger seizures. Be sure to get adequate rest every night.
- Wear a medical alert bracelet. This will help emergency personnel know how to treat you correctly if you have another seizure.
- Be active. Exercising and being active may help keep you physically fit, maintain a healthy weight and reduce depression. Make sure to drink enough water and rest if you get tired during exercise.
- Make healthy life choices. Managing stress, limiting alcoholic beverages and avoiding cigarettes, factor into a healthy lifestyle.
Personal Safety Is As Important
Seizures don’t usually result in serious injury, but if you have recurrent seizures, injury is a possibility. The following steps can help you avoid injury during a seizure:
- Take care near water. Don’t swim alone or relax in a boat without someone nearby.
- Wear a helmet for protection during activities such as bike riding or sports participation.
- Take showers instead of baths, unless someone is near you.
- Modify your furnishings. Pad sharp corners, buy furniture with rounded edges and choose chairs that have arms to keep you from falling off of them. Consider carpet with thick padding to protect you if you do fall.
- Display seizure first-aid tips in a place where people can easily see them. Include any important phone numbers there, too.
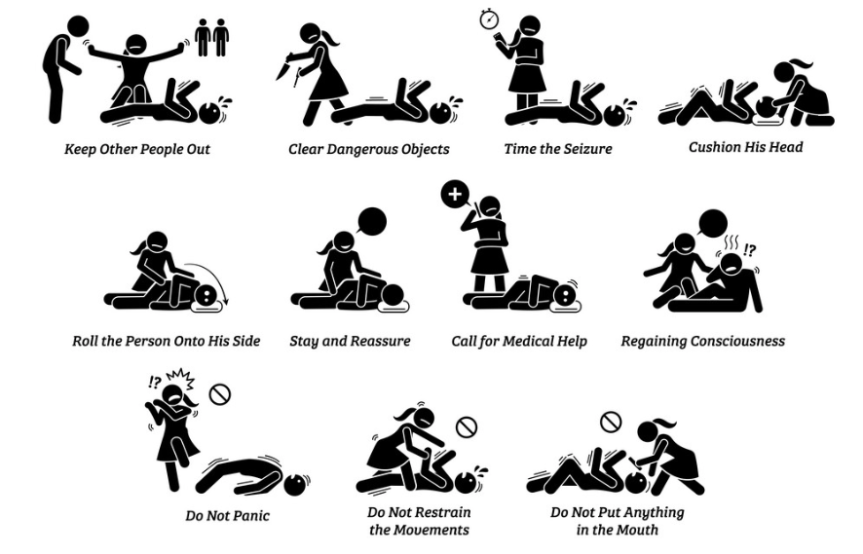
Tips On First-Aid In Case You Are A Witness To A Seizure
To help someone during a seizure, take these steps:
- Stay with the person.
- Stay calm.
- Loosen anything tight around the neck.
- DO NOT put anything in the person’s mouth viz. your finger or any object.
- DO NOT restrain the person.
- Carefully roll the person onto one side.
- Place something soft under his/her head.
- Protect from injury.
- Clear away dangerous objects if the person is moving.
- Observe the person closely so that you can provide details on what happened.
- Time the seizure.
Homoeopathy Offers A Genuine Cure
Most seizure disorders can be controlled with medication. The conventional approach of anticonvulsant drugs may provide a quick solution, in that fits are controlled and patients are happy. However, it may just be a symptomatic control and thus short-lived. Prolonged use/administration of these AEDs may have adverse effects, viz., behavioral changes, mood alterations, migraines, tremors, hair loss or unwanted hair growth, coordination disturbances (ataxia, dysarthria, diplopia), cognitive deficits, and sexual disorders (loss of libido, erectile dysfunction).
Although the seizure attacks in the girl mentioned above have come down to almost none in the last 8-10 months and we have tapered off her anti-epileptic medication, we are still struggling with the remnant coordination and behavioral issues..
Seizures represent the means whereby the body is exteriorizing an underlying condition. If we just suppress the external symptom, the disease might either find another external outlet (chronic skin issues, diarrhoea, etc.) or start to involve the deeper, more vital organs of the body.
Seizures are the acute manifestation of an underlying chronic dyscrasia, and the latter must be addressed if there has to be a successful cure.
Homoeopathy offers a genuine cure in majority of cases without any side effects. It’s not habit-forming and can be given in conjunction with conventional anti-epileptics. Each case is treated as an individual, and “tailor-made” remedies are selected on causation, signs and symptoms, factors that modify the intensity of the symptoms and their concomitants.
A miasmatic tendency (predisposition/susceptibility) of the person is also often taken into account for individualization to complete a cure.
Homoeopathic Remedies found Most Effective in Seizures
A few of the stalwart remedies used in Homoeopathy to treat epilepsy are:
- Cicuta Virosa: This homoeopathic medicine is effectively used to treat cases of epilepsy marked by violent body distortions. These can include the horrific backward bending of the spine, making the person’s face turn blue, or trigger a locked jaw. Best to treat epilepsy triggered by head injuries and worms.
- Causticum: Useful in Petit mal, esp. menstrual epilepsy occurring around puberty.
- Belladonna: In recent cases of epilepsy only. The convulsions begin in the upper extremities and extend to the face, eyes and mouth; fits of short duration several times during the day that pass off suddenly.
- Artemisia Vulgaris: Often used to treat cases of petit mal epilepsy, characterized by staring into space, leaning forwards or backwards, and stopping in a sentence abruptly. It also addresses the fear triggering the attack.
- Stramonium: Convulsions are triggered by exposure to bright lights or shiny objects, with or without loss of consciousness. The patient generally experiences jerks in the muscles of the upper body.
- Cuprum Met: Seizures preceded by an aura in the knees. Other symptoms can be spasms that begin in the fingers and toes and gradually spread to the rest of the body with jerking of muscles. This can also be used to treat convulsions that accompany menstruation and follow the delivery of a baby.
- Bufo Rana: Epileptic attacks occur in sleep, often accompanied by an aura in the genitals. This is especially helpful for women who experience seizures during menstruation.
- Hyoscyamus: Epileptic fits that are followed by deep sleep. Other symptoms are fidgeting with bedclothes, fidgeting with fingers, and muscular twitching.
- Plumbum Met: The attack is preceded by a sense of heaviness or paralysis in the legs; epileptic seizures from sclerosis, or tumors of the brain, with a gradual return of consciousness after an attack.
- Nux vomica: It suits cases arising from an excess of reflex action caused, for instance, by indigestion. The aura starts in the solar plexus, with a characteristic sensation of ants crawling over the face.
- Oenanthe Crocata: Sudden and complete loss of consciousness; swollen livid face; frothing at the mouth; dilated or irregular pupils; convulsions with locked jaw and cold extremities. Sleeplessness, stupor and apathy after the fits and the debilitating effects of the attacks are more quickly recovered with the use of this medicine.
Although these remedies indicate their therapeutic affinity for the condition, they are not a complete and definite guide to the treatment of seizures. They need to be followed by a constitutional or a miasmatic remedy to bring about a complete cure.
Through my personal experience in handling such cases, I vouch for an improvement in seizure number, intensity, frequency and duration in most cases (including a few in pet dogs), within a short span of commencement of medication. In a treatment span of a few months to a year or two, gradually, the need for conventional antiepileptic medication gets minimised, or you may even be completely weaned off them.
Do consult your Homoeopathic Physician before starting any of the medication mentioned above.

